Viability and Dating Scan
Each ultrasound examination gives important information to the referring doctor. It is a snapshot in time. Your initial ultrasound is best performed 6-8 weeks after your last menstrual period (LMP).
At this scan we hope to:
- Confirm a pregnancy
- Confirm a normal intrauterine location. This is when the BhCG hormone levels are greater than 1000Ius – usually after 6 weeks
- Confirm viability by demonstrating the presence of fetal heart motion
- Determine the number of babies present
- If more than one baby, determine their choronicity, identical/non-identical (fraternal)
- Calculate the expected date of delivery (EDD)
- Demonstrate a cause of bleeding in early pregnancy.
All early scans will include a transabdominal scan performed through your skin and requires a full bladder. It may be necessary to perform an internal or transvaginal scan. This is done after you have emptied your bladder. These internal scans do not present any harm to your baby and usually allow better visualisation.
On transvaginal scan at 5 weeks gestation, only a gestation sac will be seen. At around 6 weeks a yolk sac will become visible. At this time a small embryo becomes apparent and when it reaches 5+mm the heart beat should be visible. Doppler is used to hear the heart beat and measure the heart rate.
The crown rump length (CRL) is the measurement taken from baby’s head to bottom. This is used to calculate the expected due date. This measurement is used to date the pregnancy up until 14 weeks.
CRL measurement
3D 10 weeks
Nuchal Translucency Scan – 12 weeks
The NT scan or 12 week scan is an ultrasound best performed in the first trimester between 11 weeks and 13 weeks 6 days. This scan is combined with a blood test that looks at 2 specific hormones of pregnancy, the free Beta hCG and PAPP-A. It is an extremely accurate non-invasive screening test that helps identify a fetus at risk for Down syndrome as well as other chromosomal conditions and some major structural abnormalities. This ultrasound screening test does not have any side effects or complications.
It will however only tell us if a fetus has an increased risk. The only way to diagnose Down syndrome or other chromosomal abnormalities is by having a diagnostic test (a CVS or amniocentesis). These tests are invasive and require a needle to be passed into the maternal abdomen and uterus and therefore carry a small risk of miscarriage.
Chromosomal abnormalities occur when there is a change in the number or structure of the chromosomes. Normally we have 46 chromosomes. We acquire 23 from our mum and 23 from our dad. They are numbered 1-22 and a pair of sex chromosomes. Boys have XY and girls XX. The most common chromosomal abnormality seen at birth is Down syndrome. These babies have an extra number 21 chromosome giving a total of 47 chromosomes.
Accredited practices
To ensure your NT scan is performed correctly, it is important that you have your scan at an accredited ultrasound practice. An NT computer program was developed by the London Fetal Medicine Foundation. This is available in Australia through the Royal College of Obstetricians and Gynaecologists. Strict auditing of sonographers and ultrasound practices is undertaken every year. This ensures that the NT scan test is being performed correctly. The sonographers at Newcastle Ultrasound for Women have full NT accreditation.
12 week NT scan advantages.
These include:
- To estimate individual risk for Trisomy 21 (Down syndrome), Trisomy 18 (Edward syndrome) and Trisomy 13 (Patau syndrome).
- More accurately date the pregnancy
- Diagnose multiple foetuses
- Diagnose early pregnancy failure
- Allow early detection of some major abnormalities including spina bifida.
NT and Down syndrome
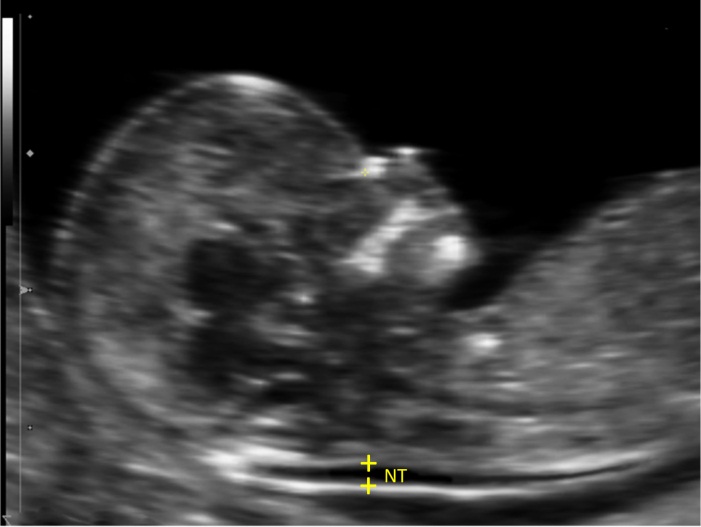
In the first trimester there is a small amount of fluid beneath the skin at the back of the neck in all fetus’s. This fluid is called the nuchal translucency (NT), and can be easily and accurately measured on ultrasound.
When there is extra fluid and the NT measurement is thicker than normal, there is an association with chromosomal anomalies such as Down syndrome or some structural abnormalities. Some babies with at thickened NT can be perfectly normal.
The fluid itself is not an abnormality and does not harm the baby but is simply a sign of a potential problem.
At the NT scan, the baby is measured from head to bottom to determine the crown-rump length (CRL) and the nuchal translucency is measured. These measurements are entered into the FMF computer program with the patient’s date of birth and the first trimester biochemistry blood test. The computer then calculates the patient’s age related risk for Down syndrome and the new individual risk for this pregnancy. The results are then discussed with the patient. The combined NT result will provide the patient with a risk assessment. This will either be a high risk result (greater than 1 in 300) or low risk (less than 1 in 300). Even with a low calculated risk, Down syndrome is not completely excluded and can still occur occasionally. Patient’s within the high risk group should then be offered further testing – NIPT, CVS or Amniocentesis.
Free BhCG and PAPP-A
Beta human chorionic gonadotrophin (free BhCG) and pregnancy associated plasma protein-A (PAPP-A) levels can be assessed from a blood test. This is best done after 9 weeks and at least a week prior to the NT scan. The BhCG tends to be higher and PAPP-A tends to be lower in pregnancies affected by Down syndrome.
Nuchal translucency accuracy
When the ultrasound is combined with the first trimester blood test and nasal bone, the detection rate increases to 95%. No screening test can give 100% detection.
Nuchal translucency measurement
The results of the NT scan will be discussed with the patient at the time of the examination.
If a pregnant woman wants to completely exclude a chromosomal abnormality, then she should consider having prenatal testing with either a CVS or an Amniocentesis.
First trimester screening for preeclampsia
Preeclampsia is an illness which only occurs in pregnancy. It is sometimes referred to as preeclamptic toxaemia, PE or PET. It usually arises during the second half of the pregnancy and can affect both the mother and her unborn baby.
Preeclampsia symptoms include:
- High blood pressure – 140/90 or greater
- Headaches
- Edema- accumulation of excess fluid especially concerning when it occurs in the face, around the eyes and in the hands
- Changes in vision- flashing lights, auras or sudden onset of blurry vision
- Protein in the urine.
In Australia, mild preeclampsia occurs in 5-10 % of pregnancies and severe preeclampsia in 1-2%.
Preeclampsia and complications associated with this condition account for 15% of direct maternal mortality and 10% of perinatal mortality.
Preeclampsia is the indication for 20% of labour inductions and 15% of Caesarean sections.
It accounts for 5-10% of preterm deliveries.
Worldwide, preeclampsia and its complications kill many tens of thousands of women and their babies every year.
In the past there was no way of screening for preeclampsia, but now screening can be performed at the 12-14 week scan. Women can be identified to be at high risk of developing the condition. The screening program can detect 90% of women who will go on to develop preeclampsia.
The advantage of early screening for preeclampsia is that early administration of low dose aspirin to the pregnant mother is now known to improve the outcomes and reduce the complications in about 50% of affected pregnancies.
A trial using asprin in early pregnancy was performed. This was the ASPRE trial: Aspirin from 12 weeks – It examined the prophylactic use of low-dose aspirin from the first trimester in women at increased risk for preterm PE. Women with singleton pregnancies had screening by means of an algorithm that combines maternal factors (previous pregnancy outcomes, weight, smoker, diabetes, hypertension, previous preeclampsia or if mother had preeclampsia), mean arterial pressure (BP), uterine artery Pulsatility index (ultrasound doppler measurement) and maternal serum placental growth factor (PlGF) and pregnancy associated plasma protein (PAPP-A) at 11-14 weeks gestation. Women with a risk for preterm preeclampsia of greater than 1:100 were invited to participate in a double-blind trial of aspirin (150mg/day) vs Placebo.
The results showed that preterm PE occurred in 1.6% of participants in the aspirin group as compared with 4.3% in the placebo group.
The incidence of PE at less than 34 weeks was reduced by 82%. The trial showed that aspirin had no significant effect in reducing the risk of term PE. The study concluded that treatment with low-dose aspirin in women at high risk for preterm PE reduced substantially the incidence of this disease.
Contraindications to aspirin use include: sensitivity to aspirin, aspirin related asthma, previous gastrointestinal sensitivity, ulcers etc.
Newcastle Ultrasound for Women now includes preeclampsia screening as part of the 12 week Nuchal scan. Referring doctors only need to ask for an NT scan on the referral form.
There is no extra cost and it is covered partially by Medicare.
No extra time is allocated to the scan.
What is involved:
- In addition to the images and measurements taken during the NT scan, a Doppler measurement of the right and left Uterine arteries is taken to obtain a PI (pulsatility index)
- The mother’s blood pressure is also taken on both arms
- Information regarding maternal factors including weight, height, previous pregnancy information, smoker, diabetes, hypertension and previous preeclampsia or family history of preeclampsia are collected.
- Added to this are some blood test results including pregnancy associated plasma protein (PAPP-A) and maternal serum placental growth factor (PlGF).
If the FTS bloods are sent to a Douglas or NSW pathology lab (Pathology North), they automatically include the PlGF measurement.
The same Fetal Maternal Foundation software that gives the risk of chromosomal abnormalities is used. By adding the PlGF, Uterine artery doppler PI measurements and the mother’s blood pressure, a risk for PE before 34 weeks, PE before 37 weeks and a Fetal growth restriction risk before 37 weeks is calculated.
Unlike the chromosomal risk which is deemed to be high when greater than 1:300 for preeclampsia the high risk group is greater than 1:100. This is printed in bold on the report.
If the blood results are available on the day of the scan, our Sonographer will discuss the Nuchal and Preeclampsia results with the patient.
If a patient chooses to have a Genesyte or Harmony NIPT, it is still essential that they also have the FTS bloods (Bhcg, PAPP-A and PlGF) so that a Preeclampsia risk assessment can be reported.
We believe every woman who chooses to have a 12-14 week scan should have preeclampsia screening included. It costs no more, is of no harm to her or the baby, and might just highlight the otherwise unknown risk of her developing preeclampsia.
To our knowledge, only a few places in Newcastle include preeclampsia screening. The sonographer performing the scan must be accredited by FMF, which runs through RANZCOG.
Non-invasive prenatal testing (NIPT)
This new technology has only been available in Australia since 2012.
NIPT is a maternal blood test that can be performed from 10 weeks gestation. It uses advanced genetic testing technology that allows for the detection and comparison of fetal DNA within the mother’s blood sample.
There is no Medicare rebate available for this test at this time. There are no risks to the baby from this test. Currently it is the most accurate screening test for Down syndrome (Trisomy 21), Edward syndrome (Trisomy 18) and Patau syndrome (Trisomy 13).
NIPT allows for a >99% detection rate for Down syndrome, a 98% rate for Edward syndrome and a 80% detection rate for Patau syndrome. There is a 93–95% detection rate for sex chromosome abnormalities including Turner syndrome and Klinefelters syndrome and >99% detection rate for fetal gender.
GeneSyte NIPT sceening test
NIPT is available for twin pregnancies and donor egg pregnancies. Gender detection is not available for twin pregnancies. This test has been validated for both high and low risk pregnancies, allowing patients to avoid the risk of miscarriage associated with the traditional invasive testing options of CVS and amniocentesis.
NIPT is not currently classified as a diagnostic test and therefore a positive result for Trisomy 21,18 or 13 will require confirmation by traditional invasive testing, CVS or amniocentesis.
If the nuchal translucency measurement is >3.5mm or there is a fetal anomaly seen on scan, even if the risk for a chromosomal abnormality is deemed to be low, then invasive testing CVS or amniocentesis should be offered.
Newcastle Ultrasound for Women recommends the GeneSyte NIPT screening test which can be performed at our Lingard practice.
19–20 Week Morphology Scan
This scan is also known as an anomaly scan and in Australia nearly all pregnancies undergo this scan at 19-20 weeks. No harmful effects of obstetric ultrasound have been shown in the past 30–40 years that it has been used routinely.
You are welcome to bring your partner or support person to the scan. The scan is used to assess:
- Placental position and cord insertion
- Cervical length
- Amniotic fluid volume
- Fetal structural development including brain, face, spine, heart, lungs, stomach, kidneys, bladder, arms, legs, hands and feet
- Fetal growth
At Newcastle Ultrasound for Women, our lovely sonographers will talk you through the scan explaining exactly what is being imaged and measured. You are welcome to ask questions.
The majority of the scan is performed using 2D imaging (black and white) which is how we check for abnormalities and measure baby’s size. A 4D scan will also be performed when the baby is in a good position for this to be done. There are limitations with the 4D scan including baby’s position and cooperation as well as maternal size. We always try to capture the best images at the time.
At the conclusion of the scan you will be provided with thermal printed images, a USB containing all the images and a DVD of the scan.
Detecting abnormalities
You will be amazed at the amount of detail that can be often seen in the morphology scan. It is important to realise however, that not all parts of the baby show up well on ultrasound. No ultrasound examination can ever guarantee a normal baby. The ultrasound scan is often limited by mum’s size, the position of the baby and an anterior placenta.
Up to half of fetal heart defects will not be seen. Most of these are only minor. Many bone growth problems, including forms of dwarfism, will only be detectable late in pregnancy or after the baby is born. Conditions such as cerebral palsy, blindness, deafness, autism and most skin and soft tissue lesions are never detected with ultrasound.
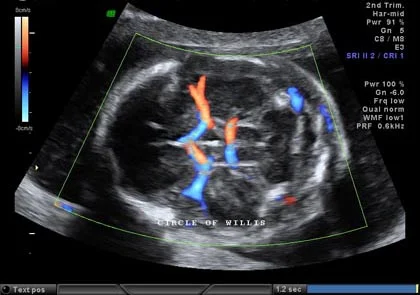
Circle of Willis
Interventricular septum
Cardiac outflow tracts
Determining the sex of your baby
We will ask if you wish to know the sex of your baby. It can be determined at this scan however ultrasound is never 100% accurate and fetal position and cooperation play a big part. We will try our best.
Third Trimester – Growth Scan
Your obstetrician may refer you for a scan in the third trimester for a number of reasons which include:
- If you have a low lying placenta on the 19–20 week scan
- If you are clinically measuring too large or too small for dates
- If you have had a small or large baby in the past
- If you have high blood pressure
- If you have diabetes or another medical condition
- If you have pain in your abdomen
- If you have had vaginal fluid loss
- If you have premature contractions
- If you are having twins etc
- If you had a low PAPP-A at NT scan
- If the umbilical artery contains only a single artery
The ultrasound will be used to assess:
- Fetal growth/size
- The amount of amniotic fluid around baby
- Doppler studies/blood flow patterns in the umbilical cord, middle cerebral artery in the brain and Ductus venosum.
- Placenta location
- Fetal well-being
Imaging the baby in the third trimester can be difficult as the baby occupies much more space in the uterus. This means in general we cannot see the baby as well as on earlier scans. The further into the pregnancy you go, the denser the bones become, which can shadow and obscure the view. This is the case when looking at the fetal brain. Things like fingers and toes, hands and feet are also more difficult to assess. The quality of the imaging depends on what position the baby is in and how cooperative the baby wants to be for us. The amount of amniotic fluid also affects the quality of the scan, more fluid is better. If there is enough fluid in front of the fetal face amazing 4D images are possible.
Assessing fetal well-being.
Ultrasound is a major tool used to assess the fetal health by using Doppler assessment and evaluating the fetal biophysical profile.
The ultrasound biophysical profile is a test that attempts to gauge whether or not the fetus is getting too little oxygen – fetal hypoxia. The sonographer examines fetal movement, breathing movement, tone, amniotic fluid volume and heart rate variability.
The baby has a number of mechanisms for coping with placental insufficiency. These include:
- Diverting blood flow to the brain and away from the kidneys and bowel. This then reduces the amount of urine and therefore the amniotic fluid around baby. The blood flows through the brain at reduced resistance and this can be measured using Doppler to assess the flow in the middle cerebral artery.
- When there is a significant problem with placental function there tends to be a decline in fetal movements. Initially, fetal chest or breathing movements disappear followed by limb and trunk movements.
- Placental function can also be assessed by examining the blood flow through the umbilical cord artery. Increasing resistance to flow will initially be reflected in the cord Doppler readings showing a high resistance waveform. In severe cases this is followed by absent or reverse flow in the artery during diastole.
Twin Pregnancy
There are different types of twin pregnancies with some being more high risk.
Dichorionic diamniotic (DCDA) twins
DCDA twins can also be called fraternal twins. The most likely scenario is 2 separate eggs are fertilized by 2 separate sperm. They are usually non-identical however approximately 10% may be identical if infact they are from one embryo which split very early in development.
DCDA twins
DCDA twins have two placentas and two separate amniotic sacs. These babies will have different genetic material.
DCDA twins are usually scanned monthly to assess growth and well being of each baby as well as to check cervical length.
Monochorionic diamniotic (MCDA) twins
Monochorionic twins occur when 1 egg and 1 sperm and therefore 1 embryo split to make 2 very early in development.
These babies therefore have identical genetic material and are identical in appearance.
MCDA twins
MCDA twins have a single placenta and 2 separate amniotic sacs.
MCDA twins are routinely scanned every 2 weeks from 16-32 weeks to monitor for evidence of twin-twin transfusion syndrome.
They are also monitored closely for growth, well being and maternal cervix length.
Monochorionic monoamniotic (MCMA) twins
MCMA twins have a single placenta and both babies share the same amniotic sac. They are identical and share the same genetic material.
MCMA twins are usually scanned weekly from 24 weeks until delivery – usually at 32 weeks. MCMA twins are at a greater risk for:
MCMA twins
- Twin-twin transfusion
- Cord entanglement and loss of one or both twins
- Conjoined twins
4D Ultrasound
A 4D scan will also be performed when the baby is in a good position for this to be done. There are limitations with the 4D scan including baby’s position and cooperation as well as maternal size. We always try to capture the best images at the time.